By Mabel Adinya Ade
Breastfeeding Week is more than a symbolic occasion; it is a powerful reminder of the foundational role that breastfeeding plays in shaping the health, development, and resilience of our children and their mothers. For Nigeria, where multiple humanitarian and socio-economic crises converge, the act of breastfeeding has become both a survival strategy and a national development priority.
Mothers who breastfeed exclusively for the first six months and continue alongside complementary feeding offer their children a solid head start in life. Breastfeeding not only reduces the risk of childhood illness and malnutrition but also empowers the mother by naturally aiding birth spacing and allowing her body to heal. Yet, for many Nigerian mothers, especially those in conflict-affected zones such as Borno in the Northeast and Benue in the Middle Belt, this natural, life-saving act is under siege.
A Crisis within a Crisis: Food Insecurity and Maternal Malnutrition
According to UNICEF, only 29% of Nigerian infants are exclusively breastfed, while the country holds the grim record of housing the highest number of malnourished children in the world. Behind this figure is a deeper crisis: the widespread malnutrition of mothers, particularly among pregnant and lactating women in internally displaced persons (IDP) camps.

In Benue State, the population of IDPs has drastically increased in recent months due to intensified attacks on rural farming communities. Camps are overcrowded with pregnant women, nursing mothers, and children under five, many of whom lack access to basic food supplies, health services, or safe shelter. These conditions are replicated in Borno State, where persistent conflict has displaced millions and left maternal health services overstretched or non-existent.
How can a malnourished mother breastfeed adequately? How can a mother living with HIV/AIDS, who is also nutritionally deprived, sustain exclusive breastfeeding? How can women in IDP camps or remote villages access safe alternatives to breastfeeding, such as therapeutic milk or infant formula, when food insecurity and inflation render even basic meals a luxury?
The Data Behind the Reality
14 million women in Nigeria suffer from micronutrient deficiency, severely undermining pregnancy and lactation outcomes.
1 in 2 pregnant women is anaemic, leading to increased risk of preterm birth and low birth weight.
Over 3.1 million Nigerians are displaced, with 1.6 million in Benue State alone.Only 19% of Nigerian children aged 6–23 months meet the minimum acceptable diet.
15 times higher risk of death exists in infants who are not breastfed compared to those who are.
150,000 HIV-positive women give birth each year, with limited access to HIV-sensitive infant feeding programs.
The National and Long-term Implications
When breastfeeding is compromised, the result is more than just a public health failure—it becomes a national development issue. Poor nutrition in early childhood is linked to irreversible cognitive delays, poor academic performance, reduced economic productivity, and increased health care burdens. For mothers, the consequences include weakened immunity, higher maternal mortality, and socio-economic vulnerability.
The failure to protect and promote breastfeeding, especially in emergency contexts like those in Borno and Benue, erodes our collective investment in future generations.
What Must Be Done
To enhance breastfeeding outcomes and safeguard maternal nutrition, especially in humanitarian and food-insecure settings, the following multi-tiered actions are necessary:
Policy & Investment
Prioritise exclusive breastfeeding and complementary feeding in national and sub-national nutrition and emergency response plans.
Invest in food and micronutrient supplementation for pregnant and lactating mothers, especially in IDP camps and rural communities.
Scale up implementation of the Baby-Friendly Hospital Initiative and enforce breastfeeding-friendly workplace policies.
Extend paid maternity leave to six months and support community-based breastfeeding counselling.
Emergency Response
Integrate Infant and Young Child Feeding in Emergencies (IYCF-E) into humanitarian responses in Benue, Borno, and other affected states.
Provide ready-to-use infant formulas and therapeutic foods in safe, monitored environments for mothers who cannot breastfeed.
Establish safe, private spaces for breastfeeding in IDP camps and health centres.
Equity & Inclusion
Design HIV-sensitive infant feeding programs to support mothers living with HIV in line with WHO and national guidelines.
Develop targeted outreach for rural women, displaced persons, adolescent mothers, and those with disabilities who face unique breastfeeding challenges.
Accountability & Advocacy
Mobilise community and faith-based organisations to promote breastfeeding education and stigma reduction.
Strengthen data collection and monitoring to ensure that investments reach the most at-risk mothers and children.
Advocate for stronger nutrition financing in both federal and state budgets.
Breastfeeding is not just a personal choice, it is a public good and a human right. In a country where maternal and child survival remains a struggle, supporting breastfeeding is one of the most cost-effective strategies to build a healthier, more prosperous Nigeria. This World Breastfeeding Week, let us rise in solidarity with mothers in Borno, Benue, and beyond, ensuring they are nourished, supported, and empowered to give their children the best start in life.
Mabel Adinya Ade
Executive Director
Adinya Arise Foundation (AAF)
8. Eket Close, Area 8, Garki, Abuja -FCT


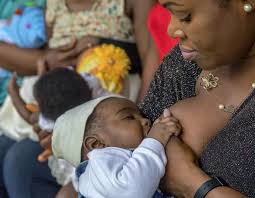






Breastfeeding saves lives, yet many Nigerian mothers—especially in crisis zones like Borno and Benue—struggle to do it safely. It’s time we prioritize maternal nutrition and support; our future depends on it.